|
8/25/2023 0 Comments Alveolar dead space in emphysemaLastly, we address one of the most commonly encountered clinical dilemmas: attempting to differentiate COPD and asthma at the bedside thus the chapter ends with a discussion on interpretation of spirometry results at baseline and with pharmacologic intervention in order to differentiate these diseases. We further compare and contrast the features of normal aging, COPD, and IPF to better understand the similarities and dissimilarities. This chapter deals with changes in (1) structure of the lung and chest wall, (2) lung volumes and lung capacities, and (3) respiratory mechanics. The term “accelerated aging” is often encountered in studies of these chronic diseases in older adults so we try here to describe the changes in the respiratory system that occur in a healthy, nonsmoking individual as a result of age and compare them with the changes indicative of chronic diseases in older adults. Cigarette smoke, accounting for the greatest population impact on the respiratory system, produces effects similar to aging and this is reflected in disease processes such as chronic obstructive pulmonary disease (COPD) and idiopathic pulmonary fibrosis (IPF). Intrinsic aging alone produces changes, but there are also consequences of lifetime accumulation of insults by environmental factors and recovery from such insults. It is imperative to understand the changes that occur in the respiratory system with age because many disease processes have a direct correlation with age-related changes in respiratory physiology. Since FEV 1/FVC values below 0.65 are typically indicative of airway obstruction, this parameter may overestimate obstructive disease in extreme old age. Though total lung capacity (TLC), made up of the two components of vital capacity (VC) and residual volume (RV), does not change with age, age-related changes in lung physiology, bone, and muscle result in decreased VC with a corresponding increase in RV as measured by standard spirometry.Īging results in a loss in forced expiratory volume in 1 second (FEV 1) of about one-third liter per decade, and the decline in FEV 1 with aging is greater than the decline in total forced vital capacity (FVC). Anatomic dead space is the volume of gas within the conducting zone (as opposed to the transitional and. DEAD SPACE: the opposite of a shunt, dead space is an area with ventilation (V) but no perfusion (Q). Physiologic or total dead space is the sum of anatomic dead space and alveolar dead space. V the amount of air that reaches the alveoli. The mean maximal inspiratory pressure (MIP) is associated with decreased handgrip strength, lower body mass index, and current smoking status for healthy 85-year-old men, it is approximately 30% lower than that of 65-year-old men. Dead space is the volume of a breath that does not participate in gas exchange. This causes reduced lung recoil, and increases dead space impairing gas exchange. Ventilation may exceed perfusion in parts of the lung resulting in increased physiological dead air space.Age-related changes within alveoli account for “senile emphysema” characterized by alveolar dilatation without destructive changes to the alveolar walls. Air may reach the periphery of the lungs but fail to make contact with the capillary blood. The alveoli become permanently damaged (see video above).This is why breathlessness and fatigue are common symptoms of COPD. This extra effort can make the patient feel very tired. However, this does not mean that your oxygen levels are low because the breathing muscles around the chest are working harder to compensate. Age-related changes within alveoli account for senile emphysema. The respiratory muscles then have to work harder to get air in and out of your lungs.As the lungs become hyper-inflated they elongate and flatten, which means the diaphragm does not work as well as it should. 
As a result, air gets trapped in the lungs and the lungs get bigger (hyper-inflated). These changes cause the air sacs (alveoli) to close before you have fully exhaled. Some hypercapnic, hypoxemic patients with COPD. Alveolar wall destruction with formation of emphysematous blebs and bullae leads to loss of gas exchanging surface (also known as increased physiologic dead space). dead space ventilation and diminished alveolar ventilation, which contributes to CO2 retention 3. In emphysema, exposure to an irritant over many years causes an inflammation in the lungs which causes the following changes: The destruction of alveolar walls causes loss of elastic recoil, early airway closure during exhalation, and air trapping in the distal air spaces. 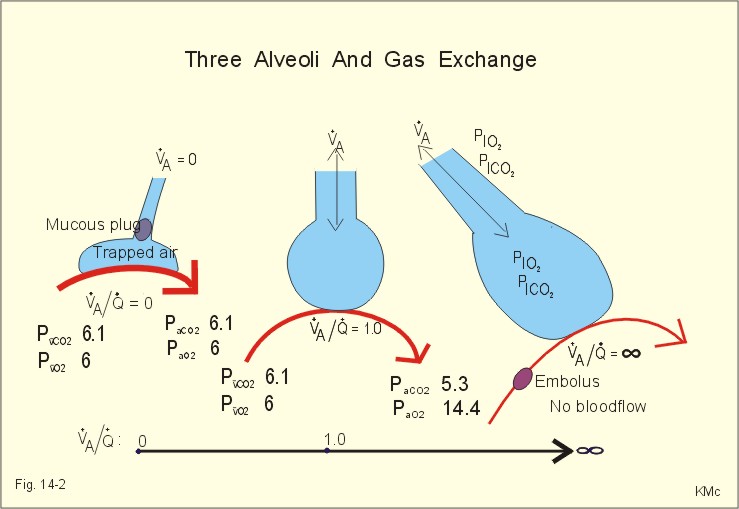
Please note there is no audio for this animation
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
